Rev Cycle Differently Denials by the Numbers
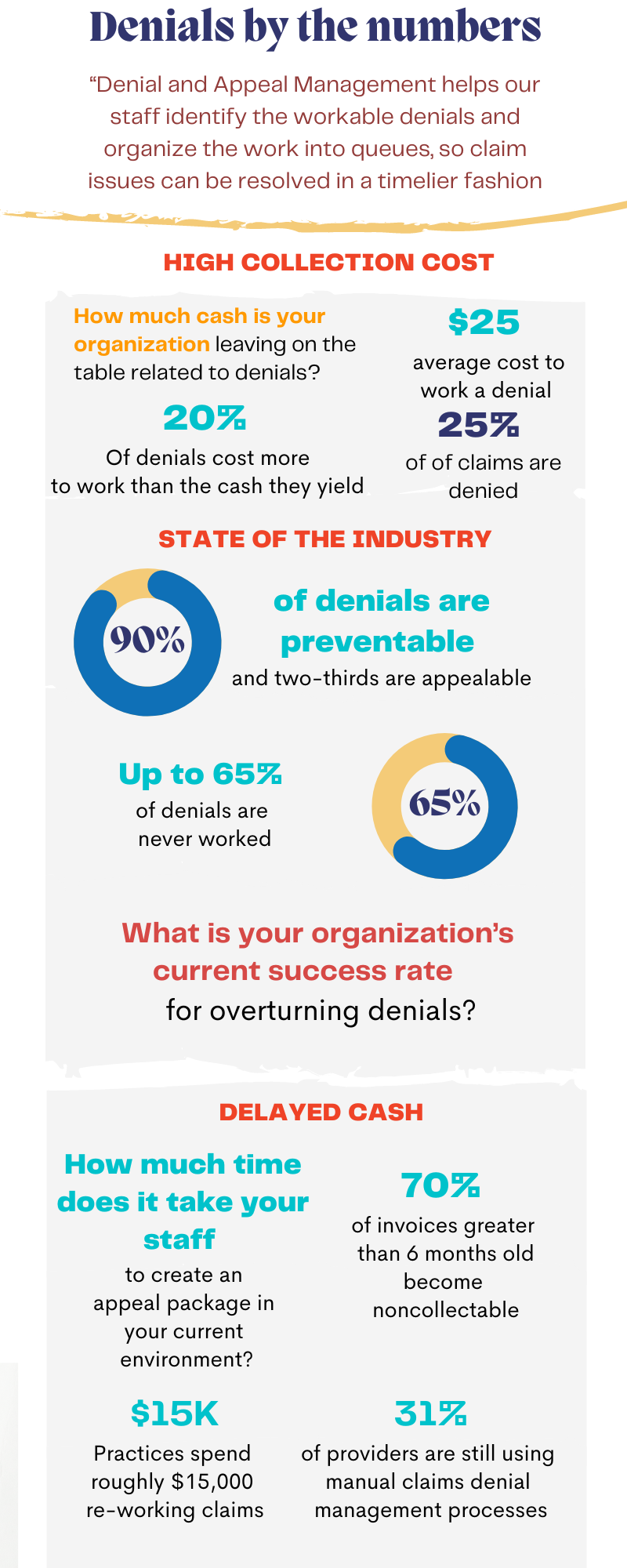
This Denial and Appeal Management helps our staff identify the workable Denial and Appeal Management.
OmniMD is a leading provider of all in one electronic health records ( ehr ) practice management ( pm ) and revenue cycle management ( rcm ) solutions and services for medical practices we have partnered with large and small medical practices medical management organizations and medical billing companies to improve patient and provider experience optimize operations and maximize financial health.
BusinessArticles from Mitesh Patel
View blog
Medical billing is a complex but essential part of the healthcare industry, and the best medical bil ...
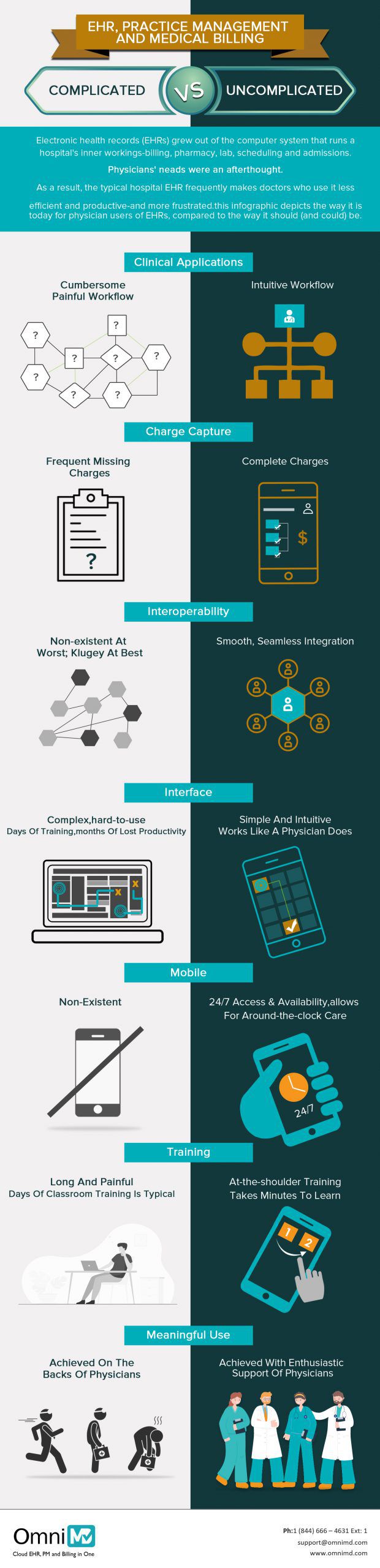
In this infographic, We provide brief details of what is complicated and uncomplicated things are in ...
You may be interested in these jobs
-

Store Operation Associate
Found in: Lensa US P 2 C2 - 1 week ago
At Home Stores LLC Fenton, United StatesJob Description$ /hourThe Store Operations Associate is responsible for unloading, processing, and stocking freight safely and efficiently to maximize product availability for the customer.Key Roles and ResponsibilitiesProvides customers a positive shopping experiencePerforms cas ...
-

Retail Cleaner
Found in: Betterteam US S2 T2 - 1 week ago
ABM Anchorage, United States Part timeABM, a leading provider of integrated facility solutions, is looking for a part-time retail store cleaner. · In this fast-paced environment your commitment to excellence will enable you to provide excellent customer service. You will be working for ABM - a company that has a true ...
-
AMI Engineer
Found in: Appcast US C2 - 1 day ago
ICONMA Baltimore, United StatesRequirements: · Required to have a bachelors degree or equivalent experience and a minimum of 5 years engineering experience performing program and technical tasks in support of nuclear plant operations. · Responsible for preparing and revising engineering documents with minima ...
Comments